 In order to find out the reason why the pacemaker was not working, pacemaker interrogation was performed immediately. An isoproterenol infusion and intravenous magnesium sulfate(MgSO4) treatment was initiated. Cardiac biomarkers, liver and renal function were normal. Laboratory analysis showed blood potassium 5.0 mmol/L and blood calcium 2.19 mmol/L. 2), we observed third-degree AV block with QT interval prolongation, and the premature ventricular contraction(PVC) was accompanied by torsade de pointes(TdP). During monitorization and ECG examination (Fig. Physical examination revealed blood pressure of 86/40 mmHg, the body temperature was 38 degree Celsius. On arrival, the patient was generalized weakness. She had a history of hypertension and was prescribed aspirin, amlodipine as regular oral medications. She was bedridden because of stroke sequelae and loss of pacemaker follow-up for the last 2 years. The patient received a pacemaker (DDDR, Cylos DR, Biotronik) due to third-degree atrioventricular(AV) block 9 years ago. 1b), and at the same time, the symptoms of the patients were immediately disappeared, NT-proBNP decreased to 347 pg/ml.Īn 80-year-old woman was admitted to our ED with fever and syncope. After the replacement of the generator, ECG showed atrial pacing at a rate of 62 bpm followed by a spontaneous ventricular rhythm (Fig. 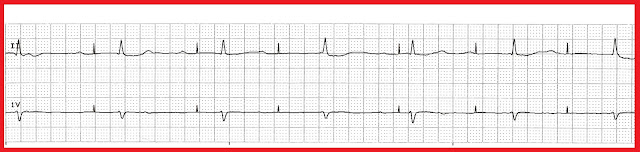
Therefore, we concluded that the patient’s symptoms corresponded to pacemaker syndrome, which included absence of rate response to physiological need, loss of atrioventricular synchrony and retrograde ventriculoatrial conduction. Soon after, pacemaker interrogation was performed with automatic reprogramming was triggered by an alert for ERI, with changes in the pacing mode (from DDDR to VVI) and the pacing rate, which was fixed at 65 bpm. 
Treatments such as anti-angina and diuretic therapy did not ease the symptoms. The echocardiography showed tricuspid moderate regurgitation, aortic valve calcification with mild insufficiency, left ventricular ejection fraction(LVEF) was 50%. The electrocardiogram (ECG) demonstrated right ventricular pacing at a rate of 65 beats/min, and retrograde P waves can be seen, indicating atrioventricular dyssynchrony. In ED, the patient was awake, his blood pressure was 146/79 mmHg, heart rate 65 bpm with regular rhythm, and lower limbs mild edema. He had not followed up with the pacemaker in the past 3 years. A new generator (DDDR, ADDR01, Medtronic) was replaced because of the pacemaker battery depletion 8 years ago. He received a pacemaker due to sick sinus syndrome. He had a past medical history of coronary heart disease and hypertension. Therefore, early detection and diagnosis is especially important.Īn 83-year-old male was admitted to our ED due to angina pectoris and dyspnea. Those cases emphasize that serious morbidity can arise from pacemaker battery depletion, even in the early stages. In addition, we introduce a method that can easily identify the depletion of the pacemaker battery, which has clinical promotion value of a certain degree. While case 2 was an 80-year-old female with complete atrioventricular heart block and torsade de pointes, due to complete depletion of pacemaker battery. 
Automatic reprogramming after pacemaker battery depletion resulted in pacemaker syndrome. Case 1 was an 83-year-old male manifesting chest pain and dyspnea. We described two cases of pacemaker battery depletion. To raise the level of awareness towards this clinical situation, we report two cases. The clinical symptoms and adverse events caused by pacemaker battery depletion are not uncommon, but it is easy to miss or misdiagnose them clinically. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
